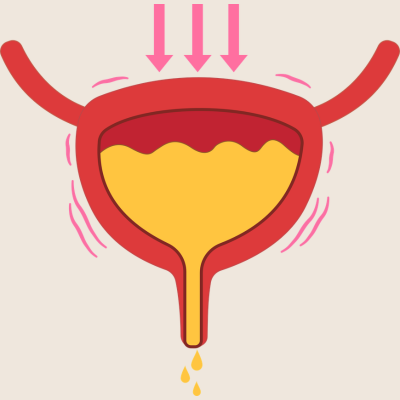
Why Do I Leak Urine When I Cough, Sneeze or Exercise?
Leaking urine when you cough, sneeze, laugh, or exercise is one of the most common pelvic health symptoms women experience, and one of the most under-reported. This article explains exactly what causes it, what is happening in your body when it occurs, and what the evidence says about treating it effectively. Whether you have recently noticed a few drops when you run or have been managing this in silence for years, understanding it is the first step to doing something about it.
Understanding the mechanics of urine leakage during physical stress
What Is Stress Urinary Incontinence?
This section defines stress urinary incontinence clearly so you know exactly what you are dealing with. Naming something is the beginning of understanding it.
Stress urinary incontinence (SUI) is the involuntary loss of urine that occurs in response to physical activity or exertion. The word "stress" here does not refer to emotional stress, it refers to physical stress placed on the bladder, bladder neck and pelvic floor. When that physical stress exceeds what the body can contain, urine leaks.
It is worth distinguishing stress incontinence from other forms of urinary incontinence, because the distinction genuinely matters for treatment. Urge incontinence involves a sudden, overwhelming need to urinate that cannot always be held back, driven by an overactive bladder. Mixed incontinence involves elements of both. Stress incontinence is specifically and directly triggered by physical exertion (coughing, sneezing, laughing, jumping, running, lifting) with no urgency necessarily involved.
Coughing and sneezing generate sharp, sudden spikes in pressure inside the abdomen. Exercise, particularly higher-impact activities like running, jumping, and HIIT training, creates repeated cycles of that pressure. Each of these events challenges the body's ability to keep the urethra sealed. When this sealing mechanism is compromised, leakage follows.
Stress incontinence is far more prevalent than most women realise. Research consistently indicates that it affects between one in three and one in two women at some point in their lives, with higher rates in women who have had children and in the postmenopausal population. The fact that so many women manage this quietly, adjusting their activities, wearing pads, avoiding certain exercises, means the true scale of the problem is almost certainly underestimated.
How Pressure Causes Urine Leakage
Understanding how leakage actually happens physically helps explain why certain activities trigger it and why the right treatment works.
Every time you cough or sneeze, there is a rapid and forceful sharp spike in intra-abdominal pressure. The pressure within the cavity of your abdomen and pelvis. This pressure is transmitted directly downward onto the bladder if not managed well. Exercise, particularly impact activity, creates repeated cycles of this same increased pressure, though typically less acutely than a single cough or sneeze.
Under normal circumstances, the bladder and urethra work together to maintain continence. The urethra is kept closed by the urethral sphincter, a ring of muscle, and by the support provided by the pelvic floor beneath it. The pressure inside the urethra, known as urethral closure pressure, must remain higher than the pressure inside the bladder for urine to stay in. When this balance is maintained, you stay dry even during physical activity.
Stress incontinence occurs when a pressure spike overwhelms the urethral sphincter's ability to maintain closure. If the sphincter is weakened, if the pelvic floor support beneath the urethra has been compromised, or if the urethra cannot close firmly enough to match the incoming pressure, the seal breaks momentarily and urine escapes. The amount that leaks depends on the intensity of the pressure spike and the degree of sphincter and pelvic floor compromise.
The relationship between bladder pressure and urethral closure pressure is central to understanding why treatment works. Anything that strengthens the structures that support the urethra, particularly the pelvic floor muscles, restores that pressure balance and reduces or eliminates leakage. This is why pelvic floor rehabilitation is so effective, and why it is the first-line treatment recommended by clinical guidelines.
The Role of the Pelvic Floor Muscles in Bladder Control
The pelvic floor is not just a supporting structure. It is an active, dynamic system that plays a critical role in maintaining continence. Understanding its role helps explain both why leakage happens and why targeted exercise works.
The pelvic floor is a group of muscles, ligaments, and connective tissue that forms the base of the pelvis in a bowl-like shape. It supports the bladder, uterus, and bowel, and it plays a direct role in urethral closure. Crucially, healthy pelvic floor muscles do not just sit passively beneath the bladder, they reflexively contract in anticipation of and in response to sudden pressure events like coughs and sneezes as well as functional tasks such as heel strike when walking. This co-contraction acts as a dynamic brace, compressing the urethra and maintaining closure at exactly the moment it is most under pressure.
When pelvic floor muscles are functioning well, this reflexive response is automatic and effective. Most women are completely unaware of it happening because it works without conscious thought. The problem arises when this reflex is delayed, insufficient (or absent), when the muscles are too weak, too poorly coordinated, or too damaged to generate the closing force needed at the moment the pressure arrives.
The consequences of pelvic floor weakness on bladder control are direct and measurable. Without adequate support beneath the urethra, the bladder neck descends under pressure, the urethra cannot seal fully, and urine escapes. This is sometimes described as hypermobility of the urethra.
Muscle function can deteriorate gradually over time, making stress incontinence feel like something that just crept up. A woman may notice that a cough occasionally causes a small leak, then more frequently, then with lighter activities like brisk walking or stair climbing. Each step in this progression reflects increasing pelvic floor compromise, and each step is also reversible with the right rehabilitation.
Recognising the Symptoms of Stress Incontinence
Recognising stress incontinence for what it is rather than dismissing it as "just one of those things" is important, because it empowers you to take action.
The hallmark symptom is leakage of urine during or immediately after physical exertion. This might mean a few drops when you cough or sneeze, a small leak when you laugh loudly, or a more significant loss when you run, jump, do jumping jacks, or lift something heavy. The leakage is directly linked to the physical event, there is typically no warning sensation before it happens, and no sense of urgency beforehand.
Symptoms vary considerably in severity. At the milder end, a woman might notice occasional leakage only during intense exercise or a forceful sneeze. At the more significant end, leakage may occur with any activity that increases abdominal pressure, including gentle walking, standing up quickly, or bending over. Neither end of this spectrum is something you simply have to manage around, but the severity does inform the treatment approach.
The most important distinction to make is between stress incontinence and urgency incontinence. If you leak without any immediate physical trigger, if the urge arrives suddenly and you cannot hold on to reach the toilet, that points more toward urgency incontinence or overactive bladder. Many women have elements of both, which is called mixed incontinence. An accurate understanding of which type you are experiencing helps direct the right treatment.
The impact of stress incontinence on daily life is frequently underestimated. Women modify their exercise routines, avoid trampoline parks with their children, wear pads as a matter of course, and feel anxious about laughing too hard in public. This quiet adjustment is understandable, but it is also unnecessary, because the condition is highly treatable and the activities you love are within reach again.
Causes and risk factors behind urine leakage when coughing, sneezing or exercising
Pelvic Floor Weakness as the Primary Cause
Pelvic floor weakness is the central mechanism through which stress incontinence develops, and understanding how it arises makes the treatment logic clear.
Weakened pelvic floor muscles reduce the support available to the bladder neck and urethra. Without that support, the structural integrity of the continence mechanism is compromised. During any activity that raises intra-abdominal pressure, the urethra cannot be held firmly closed, and leakage occurs. The degree of weakness directly correlates with the severity of symptoms, mild weakness may produce only occasional leakage during significant exertion, while more pronounced weakness can result in leakage during everyday movements.
Pelvic floor weakness rarely develops overnight. It is usually the cumulative result of one or more contributing factors e.g. childbirth, hormonal changes, repeated straining, high-impact exercise, without adequate pelvic floor rehabilitation. Recognising the contributing factors in your own situation helps target rehabilitation effectively.
Childbirth and Pregnancy
Childbirth is the single most significant risk factor for stress urinary incontinence in women, and understanding what happens to the pelvic floor during this time can help remove any sense of shame or confusion about why symptoms have developed.
Vaginal delivery places enormous mechanical strain on the pelvic floor. The muscles, fascia, and connective tissue are stretched far beyond their resting capacity during the second stage of labour, and in many cases there is direct trauma (tearing, episiotomy, or nerve damage) that compromises the pelvic floor's structural integrity. Studies using imaging have shown that the levator ani muscle (the primary supporting muscle of the pelvic floor) can sustain visible avulsion injuries (partial or complete detachment) during vaginal delivery. These injuries do not always cause immediate symptoms but can contribute to stress incontinence months or years later.
Pregnancy itself also plays a role, even before delivery. As the uterus grows, intra-abdominal pressure increases progressively throughout pregnancy. The pelvic floor bears the weight of the growing baby, placenta, and uterus, and this sustained load can weaken muscle tone over the nine months of gestation. Many women begin experiencing stress incontinence during the third trimester precisely because of this.
Women who have had multiple pregnancies face a compounding risk. Each pregnancy and delivery adds to the cumulative load on the pelvic floor, and recovery between pregnancies may be incomplete if pelvic floor rehabilitation is not undertaken. This is one of the strongest arguments for postnatal pelvic floor assessment after every birth, not just the first.
The long-term effects of childbirth-related pelvic floor trauma can persist for decades if left unaddressed. Some women notice symptoms immediately postnatally; others find that stress incontinence emerges or worsens around menopause, when declining oestrogen further reduces the tissue quality that had been partially compensating for earlier damage. It is never too late to rehabilitate, and it is never "just part of having had children" that you have to accept.
Menopause and Hormonal Changes
Menopause is a significant turning point for pelvic floor health, and understanding the hormonal dimension helps explain why symptoms often change or worsen during this life stage.
Oestrogen plays a key role in maintaining the quality and elasticity of the muscles, connective tissue, and urethral lining that support continence. As oestrogen levels decline during perimenopause and menopause, these tissues become thinner, less elastic, and less able to maintain the tone and closure pressure needed to prevent leakage. The urethral lining itself depends on oestrogen as well and oestrogen depletion can directly reduce urethral closure pressure.
For women who already had some degree of pelvic floor compromise from childbirth or other factors, the hormonal changes of menopause can tip the balance, turning occasional or mild symptoms into more frequent or significant ones. This is why stress incontinence often becomes more noticeable in the perimenopausal years, even in women who felt they had "got away with it" after previous pregnancies.
Postmenopausal women are disproportionately affected by stress incontinence as a result of this combination: pre-existing structural changes from childbirth, age-related muscle changes, and oestrogen-related tissue changes converging at the same time. This is not inevitable or permanent, targeted rehabilitation (and where clinically appropriate, topical oestrogen therapy) can make a significant difference.
Obesity and Its Impact on Bladder Leakage
Body weight is a modifiable risk factor for stress incontinence and the relationship between them is direct and well-evidenced.
Excess body weight, particularly carried around the abdomen, increases the chronic resting pressure within the abdominal cavity. This means the pelvic floor is bearing greater load continuously, not just during activity. Over time, this sustained elevated pressure fatigues and weakens pelvic floor muscles and stretches the connective tissue supporting the bladder and urethra.
Obesity also compounds whatever pelvic floor weakness is already present. A woman with mild stress incontinence may find her symptoms worsen significantly with weight gain, because the increased baseline pressure means even smaller activities e.g. standing up or walking, generate enough force to cause leakage. Conversely, weight loss is one of the most evidence-supported lifestyle interventions for improving stress incontinence, with studies showing meaningful reductions in leakage episodes following modest weight reduction.
Chronic Cough and Smoking
The way you breathe and the health of your airways has a more direct connection to pelvic floor function than most people expect.
A persistent chronic cough is, in mechanical terms, a repeated high-intensity stress test for the pelvic floor. Every cough generates a sharp spike in intra-abdominal pressure, and someone with a chronic cough may cough dozens or hundreds of times per day. This repeated mechanical stress progressively weakens the pelvic floor muscles and connective tissue, contributing directly to stress incontinence over time.
Smoking is closely connected to chronic cough through its effects on the airways and lungs, and therefore associated with urinary incontinence. Beyond causing or worsening chronic cough, smoking-related tissue changes may compromise the quality of urethral and pelvic floor connective tissue. Smoking cessation is one of the lifestyle changes most likely to benefit pelvic floor health, and general health more broadly.
Constipation and Straining
Bowel health and pelvic floor health are intimately connected. A relationship that is often overlooked when addressing stress incontinence.
Chronic straining during bowel movements exerts repeated, forceful downward pressure on the pelvic floor. Over months and years, this habitual straining stretches and weakens the pelvic floor muscles and the nerve supply to the pelvic floor, contributing to the muscle weakness that underlies stress incontinence. In this way, untreated constipation actively undermines pelvic floor rehabilitation efforts.
Constipation also increases resting intra-abdominal pressure due to a full bowel, adding to the chronic load on the pelvic floor. Addressing constipation through adequate hydration, dietary fibre, appropriate positioning on the toilet (feet raised on a small stool to align the bowel), and bowel habits is an important and often underemphasised component of managing stress incontinence.
Age-Related Muscle Weakness
Ageing affects muscle tissue throughout the body, and the pelvic floor is no exception.
From around the mid-thirties onwards, there is a natural, gradual decline in overall muscle mass and tone if active steps are not taken to maintain it. This process, known as sarcopenia, affects the pelvic floor muscles as it does all others. The urethral sphincter also loses some functional capacity with age, reducing its ability to generate the closure pressure needed to resist physical stress.
The cumulative effect is that older adults, and particularly older women, given the additional contributions of childbirth and oestrogen decline, experience more frequent bladder leaks during physical activity. But age is not destiny. The pelvic floor responds to targeted exercise at any age, and significant improvements in bladder control are achievable well into later life. Many clients in their sixties and seventies experience transformative results from pelvic floor rehabilitation that they had assumed was simply no longer possible for them.
Diagnosis, Treatment, and Management of Stress Urinary Incontinence
Assessment and Diagnosis
Getting an accurate assessment is the foundation of effective treatment. It ensures you receive care targeted at your specific situation rather than a generic response.
Healthcare providers assess stress incontinence through a combination of clinical history, physical examination, and sometimes specialist investigations. A thorough history will explore the nature of your symptoms, when leakage occurs, how much leakage there is, and what activities trigger it. It will also explore relevant history including pregnancies and deliveries, surgical history, bowel function, and any medications that might affect bladder function.
A bladder diary by means of recording fluid intake, urination times, and leakage episodes over several days, is an enormously useful diagnostic tool. It reveals patterns that are not always apparent from history alone, and it provides a baseline against which to measure treatment progress. A physical examination will typically include an assessment of pelvic floor muscle function, strength, coordination, endurance, and any evidence of prolapse or other structural changes. Urodynamic testing, which measures bladder and urethral pressures during filling and voiding, may be used in more complex cases or before surgical intervention.
Accurate diagnosis matters because the treatment for stress incontinence differs from that for urgency incontinence and mixed incontinence. Treating the wrong type, or not distinguishing between types, can produce poor outcomes. A specialist assessment ensures the approach is matched to the actual problem.
When should you seek help? The honest answer is: sooner rather than later. There is no threshold of severity you need to reach before your symptoms are "bad enough" to deserve professional attention. If leakage is affecting your confidence, your exercise habits, or your daily life in any way, that is enough. And if you have simply been wondering about it, come and have a conversation, there is never any judgement here, only support.
Pelvic Floor Muscle Training and Kegel Exercises
Pelvic floor muscle training is the gold-standard, first-line treatment for stress urinary incontinence and it works. This section gives you a clear understanding of how to do it effectively.
Pelvic floor muscle training targets the root cause of stress incontinence directly: it rebuilds the strength, coordination, and endurance of the muscles responsible for urethral support and closure. Multiple high-quality clinical trials have demonstrated that consistent, correctly performed pelvic floor muscle training significantly reduces or resolves stress incontinence in the majority of women who undertake it. It is recommended as the first treatment option by NICE (the National Institute for Health and Care Excellence) guidelines in the UK.
Performing Kegel exercises correctly is essential and this is where a lot of women encounter difficulty. The contraction should involve lifting and squeezing the pelvic floor inward and upward, as if you are trying to stop the flow of urine and prevent passing wind at the same time. It should not involve tightening the buttocks, holding your breath, using other muscle groups whilst you squeeze and with no bearing downward. If you are unsure whether you are doing this correctly, a pelvic floor physiotherapist can assess this directly and give you precise guidance.
For effective strengthening, the muscles need to be worked in a progressive and consistent way. A general guidance framework involves performing a mix of sustained holds (contracting and holding for several seconds before releasing) and quick flicks that train the reflex response needed during coughing and sneezing. Aim for multiple sets per day. However, the specific programme should be tailored to your current muscle function. What you need if your pelvic floor is extremely weak differs from what you need for moderate weakness or for a pelvic floor that is tight or non relaxing or poorly coordinated.
Physiotherapy-guided pelvic floor rehabilitation consistently produces better outcomes than self-directed exercise. A specialist pelvic floor physiotherapist can accurately assess your muscle function, design a programme matched to your specific needs, monitor your progress, and adjust the programme as you improve. If you have been doing ‘Kegels’ for a while without noticing improvement, it is very likely that technique, load, or frequency needs adjusting or that there are other aspects of how your body is functioning that needs addressing, not that the approach does not work for you.
Lifestyle Changes to Reduce Urine Leakage
Alongside pelvic floor rehabilitation, several lifestyle adjustments can meaningfully reduce the burden of stress incontinence and support recovery.
Weight management is one of the most impactful lifestyle changes available. Even modest weight reduction (in the range of 5 to 10 percent of body weight) has been shown in clinical studies to significantly reduce leakage episodes in women with stress incontinence. This works by reducing the chronic baseline pressure on the bladder and pelvic floor, giving rehabilitation efforts better conditions in which to succeed.
Fluid and dietary management also play a role. Staying well hydrated with plain water is important. Concentrated urine irritates the bladder lining and can worsen symptoms. Reducing caffeine, alcohol, and highly acidic foods and drinks can reduce bladder irritability. The goal is not to restrict fluids. Under-hydration can worsen symptoms so it’s important to optimise what and how you are drinking.
Addressing chronic cough through smoking cessation or appropriate medical management, and resolving constipation through diet, hydration, and positioning, removes two significant sources of repeated pelvic floor stress. These changes protect the pelvic floor during rehabilitation and prevent ongoing damage that undermines progress.
Modifying exercise during the rehabilitation phase can also be valuable. High-impact activity (running, jumping, heavy lifting) places the greatest demand on a compromised pelvic floor. This does not mean stopping exercise entirely though as staying active is important for overall health. But temporarily substituting lower-impact options while pelvic floor strength rebuilds gives the muscles a more manageable starting point, with a return to preferred activities as strength improves.
Bladder Training and Behavioural Strategies
Behavioural strategies complement pelvic floor rehabilitation and can make a meaningful difference to day-to-day management of stress incontinence.
Bladder training involves gradually extending the intervals between urinations, which helps recalibrate the brain-bladder relationship and reduces urgency-driven components of leakage. While bladder training is primarily associated with urgency incontinence, it has a role in mixed incontinence situations and supports overall bladder health and control.
Timed voiding. Going to the toilet on a schedule rather than responding to every urgency signal or visiting the toilet "just in case" helps normalise bladder habits and prevents the bladder from being trained to expect emptying at low volumes. Urge suppression strategies, including engaging the pelvic floor firmly when urgency arises and using distraction techniques, support this process.
Practically, there are also straightforward strategies that can reduce leakage during daily activities while rehabilitation progresses: bracing the pelvic floor before a cough or sneeze (the "knack" technique), engaging the pelvic floor before lifting, and choosing lower-impact exercise modifications where needed. These are not permanent workarounds but they are tools for maintaining confidence and reducing leakage while your strength improves.
Medical and Surgical Treatment Options
For most women, pelvic floor rehabilitation and lifestyle changes produce significant and lasting improvement. For some, additional medical or surgical options are part of the picture and it is helpful to understand what is available.
Medication options for stress urinary incontinence are more limited than for urgency incontinence. Duloxetine, a serotonin-norepinephrine reuptake inhibitor, is the one medication licensed in the UK for stress incontinence; it works by increasing the tone of the urethral sphincter. It can reduce leakage episodes but has side effects, and it is generally considered an option when conservative treatment has not provided adequate improvement rather than a first-line treatment. Topical oestrogen (applied vaginally) may be recommended for postmenopausal women to improve tissue quality and urethral function as well as comfort from dry and thinning tissue.
Surgical treatment for stress incontinence centres on procedures that restore urethral support. The mid-urethral sling procedure, which involves placing a small tape beneath the urethra to provide a supportive hammock, has a well-established evidence base and good long-term outcomes for appropriately selected patients. However, surgery is not a first step, nor is it a substitute for pelvic floor rehabilitation. NICE guidelines recommend that conservative management is undertaken for an adequate period before surgical options are considered.
Criteria for surgery include significant impact on quality of life, failure of conservative management despite adequate trial, and suitability following clinical assessment. Surgical outcomes for mid-urethral slings are generally positive, with the majority of women achieving continence or significant improvement. A thorough discussion with a urogynaecologist is essential to understand individual risk, benefit, and alternatives before making any decision.
Non-surgical support options include continence pessaries which are silicone devices worn internally that provide mechanical urethral support that can be useful for managing symptoms during high-impact activities or during pregnancy and postnatal recovery. These are fitted by a specialist and can be a helpful bridge while rehabilitation progresses.
Ongoing Care and Long-Term Management
Recovery from stress incontinence is not a destination you reach and then leave behind. It is an ongoing relationship with your body that, with the right habits, becomes second nature.
The pelvic floor responds to consistent, progressive exercise in the same way any other muscle group does: it strengthens with appropriate load and weakens with neglect. Women who achieve excellent results from pelvic floor rehabilitation (and that is the majority who engage with it consistently) tend to maintain those results long-term when they continue with a maintenance exercise programme. This does not mean daily clinical-level sessions indefinitely; it means integrating pelvic floor awareness and exercise into everyday life.
Regular physiotherapy check-ins, particularly during significant life transitions e.g. another pregnancy, perimenopause, a period of increased physical demands, can support long-term recovery and catch early regression before it becomes symptomatic again. Many women find that a review at these stages or with increasing symptoms gives them confidence and keeps their programme calibrated to their current needs.
A personalised management plan that combines pelvic floor exercise, lifestyle habits, and appropriate medical care is the most effective long-term framework. This plan should be built around your life, your activities, and your goals and not a generic template. Understanding your body and what it needs, and having the tools to respond to changes, is the kind of body literacy that creates lasting freedom.
If at any point your symptoms return, worsen, or change in character, that is a signal to seek reassessment rather than simply increasing exercise and hoping for the best. Changes in symptoms can reflect new contributing factors e.g. hormonal changes, a new activity, changes in weight or bowel health, that deserve proper attention. You are not starting from scratch, you are working with a body that has proven it can respond and recover.
Key Takeaways
Stress urinary incontinence, leaking urine when you cough, sneeze, or exercise, is a common, well-understood, and highly treatable condition caused by a mismatch between intra-abdominal pressure and the urethral and pelvic floor support that contains it. The primary driver is pelvic floor weakness, most often resulting from pregnancy and childbirth, hormonal changes around menopause, or the cumulative effects of ageing, straining, or high-impact activity without adequate conditioning. Pelvic floor muscle training, guided by a specialist physiotherapist, is the evidence-based first-line treatment and produces significant improvement for the majority of women who undertake it correctly and consistently. Lifestyle changes including weight management, fluid optimisation, and addressing chronic cough or constipation support and accelerate rehabilitation. If leakage is affecting your confidence, your exercise habits, or your quality of life in any way, please reach out for support. You are not alone in this, it is not something you have to accept, and the right help makes an enormous difference.